NV Billing General - Nevada Medicaid
Nov 17, 2020 · Transfer (EFT) payment policy for all new Nevada Medicaid providers and for all existing Nevada Medicaid providers upon re-enrollment Chapter 8 01/30/2009 hapter 3, “Recipient Eligibility” updates reflecting new policies that update Welfare information. hapter 8, “l aims Processing
Download NV Billing General - Nevada Medicaid
Information
Domain:
Source:
Link to this page:
Please notify us if you found a problem with this document:
Documents from same domain
NDC Billing Reference - Nevada
www.medicaid.nv.govNDC Billing Reference for Nevada Medicaid and Nevada Check Up Claims Updated 06/08/2016 (pv01/07/2014) Page 3 Form EA GM ML …
Form, Reference, Medicaid, Nevada, Billing, Ndc billing reference, Nevada medicaid
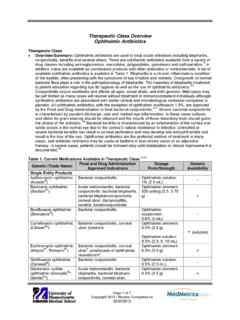
Therapeutic Class Overview Ophthalmic …
www.medicaid.nv.govTherapeutic Class Overview: ophthalmic antibiotics Page 3 of 7 Copyright 2012 • Review Completed on 02/20/2012 Generic (Trade Name) Food and Drug Administration
Antibiotic, Drug, Overview, Class, Therapeutic, Ophthalmic, Therapeutic class overview ophthalmic, Therapeutic class overview, Ophthalmic antibiotics
Behavioral Health Enrollment and Re -Enrollment …
www.medicaid.nv.govFrequently Asked Questions Revised: 12/05/2011 Provider Enrollment , Behavioral Health 1 / 6 Behavioral Health Enrollment and Re -Enrollment
Frequently, Asked, Provider, Enrollment, Frequently asked, Enrollment and re enrollment
PROVIDER QUICK REFERENCE GUIDE: Prior …
www.medicaid.nv.govNevada Medicaid/Nevada Check Up Prior Authorization Quick Reference Guide Page 1 of 4 Updated 07/24/2017 pv01/09/2015 PROVIDER QUICK REFERENCE GUIDE: Prior Authorization Requests
Guide, Reference, Provider, Nevada, Authorization, Quick, Prior, Prior authorization, Reference guide, Provider quick reference guide
CMS-1500 (version 02-12) Claim Form Instructions
www.medicaid.nv.govUpdated 07/27/2017 CMS-1500 (02-12) Claim Form Instructions pv05/18/2015 1 These instructions address Nevada Medicaid paper claim requirements. If you submit electronic claims through a clearinghouse, please contact the clearinghouse directly
Form, Instructions, Claim, Nevada, Claim form instructions, 20 21
Provider Revalidation Instructions (Individuals) - …
www.medicaid.nv.gova) Any hospital, skilled nursing facility, home health agency, independent clinical laboratory, renal disease facility, rural health clinic or health maintenance organization that participates in Medicare (Title XVIII);
Instructions, Individuals, Medicare, Provider, Home, Provider revalidation instructions, Revalidation
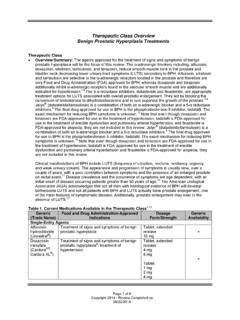
Therapeutic Class Overview Benign Prostatic …
www.medicaid.nv.gov• A systematic review of alfuzosin studies showed a greater improvement in the primary outcome (IPSS) over placebo (weighted mean difference, -1.8 points; 95% confidence interval [CI], -2.49 to -
Overview, Class, Therapeutic, Benign, Therapeutic class overview benign prostatic, Prostatic
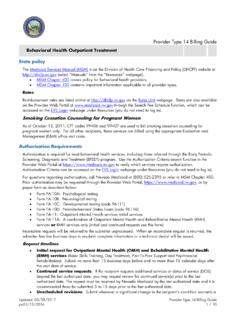
Behavioral Health Outpatient Treatment State policy
www.medicaid.nv.govProvider Type 14 Billing Guide Updated: 03/28/2017 Provider Type 14 Billing Guide pv01/15/2016 4 / 10 Behavioral Health Outpatient Treatment 96111 Developmental testing; extended (includes assessment of motor, language, social, adaptive and/or
Health, Social, States, Treatment, Behavioral, Outpatient, Behavioral health outpatient treatment state, Behavioral health outpatient treatment
A Nevada Medicaid-certified physical or …
www.medicaid.nv.govUpdated: 02/06/2013 Provider Types 30 and 83 Billing Guide pv10/01/2011 1 / 6 A Nevada Medicaid-certified physical or occupational therapist …
Certified, Medicaid, Occupational, Physical, Nevada, Therapist, Billing, Nevada medicaid certified physical or, Nevada medicaid certified physical or occupational therapist
Provider Types 20, 24 and 77 Billing Guide - …
www.medicaid.nv.govUpdated: 08/07/2018 pv04/11/2018 Provider Type 20, 24 and 77 Billing Guide Physician, M.D. and Osteopath, D.O., Advanced Practice …
Related documents
Florida Medicaid
ahca.myflorida.com2.1 Eligibility Identification and Verification An eligible recipient must be enrolled in the Florida Medicaid program on the date of service and meet the criteria provided in the appropriate service-specific coverage policy. Recipients must provide proof of eligibility when obtaining Florida Medicaid services. Florida
Eligibility, Verification, Medicaid, Florida, Florida medicaid
DSS Medical Assistance Program ELIGIBILITY RESPONSE …
www.ctdssmap.comAll Medicaid Covered Services as presented on page 1 under the eligibility response for “HUSKY ” plus specific behavioral & support services. ABI eligibility questions 1-800-445-5394 Prior Authorization Requests In addition to those listed on page 1 under the Prior Authorization Section under the eligibility response
Wisconsin Medicaid for the Elderly, Blind, or Disabled ...
www.dhs.wisconsin.govthe Medicaid program. If someone in your household is not applying for Medicaid, you do not need to provide Social Security Number (SSN) information for that person. Any person who wants Wisconsin Medicaid, but does not provide their SSN or apply for one will not be eligible for benefits, pursuant to Wis. Stat. § 49.82(2).
Behavioral Health Outpatient Treatment - Nevada Medicaid
www.medicaid.nv.govMar 18, 2022 · For questions regarding authorization, call Nevada Medicaid at (800) 525-2395 or refer to MSM Chapter 400. Prior authorization may be requested through the Provider Web Portal, https://www.medicaid.nv.gov, by using the appropriate FA form listed below: • Form FA-10A: Psychological testing • Form FA-10B: Neuropsychological testing
Health, Treatment, Medicaid, Behavioral, Nevada, Outpatient, Nevada medicaid, Behavioral health outpatient treatment
Georgia Medicaid Home & Community Based Waiver Services
www.mmis.georgia.govEligibility Verification There are three ways Georgia Medicaid provides verification of member eligibility: GAMMIS website www.mmis.georgia.gov (Username and Password is required) Interactive Voice Response System (IVRS) Provider Services Contact Center (PSCC) Contact number is 1-800-766-4456
Eligibility, Verification, Medicaid, Georgia, Mims, Eligibility verification, Georgia medicaid
The New Jersey Medicaid Program and Estate Recovery …
www.state.nj.usMedicaid beneficiaries, or former Medicaid beneficiaries, for all payments provided through the Medicaid program for services received on or after age 55 This includes, . but is not limited to, capitation payments made to any managed care organization, transportation broker, PACE provider, or any other capitatedprovider, regardless of