Explanation Of Information On Provider
Found 10 free book(s)Practitioner and Provider Compliant and Appeal Request
www.aetna.comwell as information that will support your appeal, which may include medical records, office notes, discharge summaries, lab records and/or member history (this is not an all-inclusive list) to the address listed on your Explanation of Benefits (EOB) or other correspondence received from Aetna. Please provide the following information.
Practitioner and Provider Compliant and Appeal Request
www.aetna.comwell as information that will support your appeal, which may include medical records, office notes, discharge summaries, lab records and/or member history (this is not an all-inclusive list) to the address listed on your Explanation of Benefits (EOB) or other correspondence received from Aetna. Please provide the following information.
2021 Provider Manual - Alliant Health Plans
www.alliantplans.comMember ID can be found on the Member’s Identification Card or an Explanation of Payment. Online Eligibility, Benefits, and Claim Status are available by registering for our online portal. Please see : ... 2021 Provider Manual Important Information Page | 4 ...
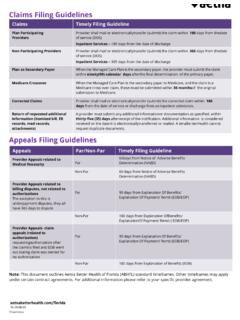
Claims Filing Guidelines
www.aetnabetterhealth.comWhen the Managed Care Plan is the secondary payer, the provider must submit the claim within : ninety (90) calendar days : after the final determination of the primary payer. ... Explanation Of Payment/ Remit (EOB/EOP) Non-Par : 180 days f rom Explanation Of Benefits/ Explanation Of Payment/ Remit (EOB/EOP) Provider Appeals- claim ...
PROVIDER TRAINING NOTICE OF MEDICARE NON …
www.meridianathome.comJul 01, 2015 · OPTIONAL: Additional Information. This section provides space for additional pertinent information that may be useful to the enrollee. It may not be used as the Detailed Explanation of Non-Coverage, even if facts pertinent to the termination decision are provided. Signature line: The beneficiary or the representative must sign this line.
2021 Provider Billing Manual - Carolina Complete Health
network.carolinacompletehealth.comgenerate an Explanation of Payment (EOP). A claim is a request for reimbursement either electronically or by paper for any medical service. A claim must be filed on the proper form, such as CMS 1500 or UB 04. A claim will be paid or denied with an explanation for the denial. For each claim processed, an EOP will be mailed to the provider who
DEPARTMENT OF HEALTH AND HUMAN SERVICES Form …
www.cms.govD. Provider Taxonomy Code (Provider Type/Specialty) and License Number Information (Required) Provide your 10-digit taxonomy code. You must select a primary taxonomy code in order to facilitate aggregate reporting of providers by classification/ specialization. If you need additional taxonomy codes to describe your type/classification ...
Connecticut Department of Social Services May 2021 TO RE ...
www.ctdssmap.comProvider Bulletin 2021-36 May 2021 page 2. Questions? Need assistance? Call the Provider Assistance Center Mon–Fri 8:00 am – 5:00 pm Toll free 1-800-842-8440 or write to Gainwell Technologies, PO Box 2991, Hartford, CT 06104 Program information is available at www.ctdssmap.com . Claims that are submitted electronically
Provider Office Manual
provider.superiorvision.comThis Provider Manual is intended to assist you and your office staff in understanding the administrative procedures related to the Superior Vision Plan. Please visit our website at www.superiorvision.com for additional information to supplement this manual. If you have any questions, please call our Provider Relations Department at
STATE OF MISSOURI MANUAL PERSONAL CARE
manuals.momed.compersonal care production : 09/24/2021 2 section 1-participant conditions of participation .....15 1.1 individuals eligible for mo healthnet, managed care or state