Wageworks Claim
Found 8 free book(s)10 Dear Ford Retiree,
media.umbraco.ioPended claim(s) If you have approved pended claim(s) at WageWorks/HealthEquity, no action is needed. The lump sum for pended claim(s) will transfer to Via Benefits on January 27, 2022. Once these claims are loaded, the pended claim(s) balance will be drawn against your new 2022 allocation and paid immediately.
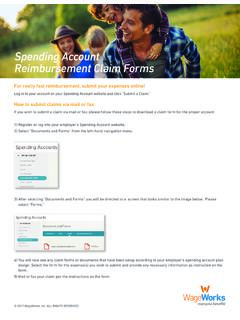
Spending Account Reimbursement Claim Forms - WageWorks
www.wageworks.com4) You will now see any claim forms or documents that have been setup according to your employer’s spending account plan design. Select the form for the expense(s) you wish to submit and provide any necessary information as instructed on the form. 5) Mail or fax your claim per the instructions on the form. Spending Account Reimbursement Claim ...
MEDICARE REIMBURSEMENT ACCOUNT CLAIMS
www.bcbsm.comSUBMITTING A CLAIM . There are four ways to submit your claim: online, via the EZ Receipts app, by fax or by mail. The method ... WageWorks is an independent company that administers the Medicare Reimbursement Account on behalf of the BCBS Service Beneft Plan.
Are you eligible for a Medicare reimbursement?
www.bcbsm.comclaim must provide proof of a Medicare Part B premium payment. Examples include: • Credit card statement • Bank statement • Social Security Cost of Living Adjustment statement or Annuity Statement Once members have proof, they can submit claims in a few different ways: • Mail or fax using this form • Online through WageWorks
2021 Benefits At-A-Glance
msh.careteamapp.comhttps://myspendingaccount.wageworks.com * Paper claims are not accepted for Trip Transit expenses Default Coverage House Staff members who do not enroll within the 30 day period will receive the following default coverage: United Health Care/UMR Traditional Plan, CVS/ Caremark prescription coverage, basic life insurance, basic
PLEASE READ THIS BEFORE SUBMITTING YOUR RETIREE …
www.wageworks.comyour claim. X Keep your original receipts, make copies — if your claim is incomplete, you will be required to resubmit the claim form and receipts. Send legible copies of your receipts. X Do not submit premium expenses on this claim form for premiums paid to your health plan if you have elected the auto-reimbursement process with Extend Health.
2020 Benefits Information for Associates Leaving Walmart
one.walmart.comWageWorks will mail you a COBRA notice and election form within 14 days after they receive notification of your termination. If you don’t receive the notice, call WageWorks at 800-570-1863. To elect COBRA continuation coverage, return the completed form to WageWorks within 60 days of the date of the notice. If you make this election and
MEDICARE REIMBURSEMENT ACCOUNT (MRA) CLAIM FORM ...
www.fepblue.orgSubmit your completed claim via toll-free fax: (877) 353-9236 OR mail: Claims Administrator, PO Box 14053 Lexington, KY 40512 I certify that the information on this form is accurate and complete. I am requesting reimbursement for Medicare Part B premium expenses I incurred while a member of the Blue Cross and Blue Shield Service Benefit Plan.