2021 Service Benefit Plan Specialty Drug List
The specialty drug list is updated monthly and is subject to change without notice. If you are a member or health-care provider and have specialty drug-specific questions, please call 1- 888-346-3731 weekdays from 7 a.m. to 9 p.m. or weekends from 8 a.m. to 6:30 p.m. Eastern time.
Tags:
Drug, Lists, Specialty, Specialty drug list
Information
Domain:
Source:
Link to this page:
Please notify us if you found a problem with this document:
Documents from same domain
BCBSMT Health Insurance Marketplace 6 Tier Drug List ...
www.myprime.comSome drugs in the same dosage form may be used to treat more than one medical condition. In these instances, ... Compounded medications: Your benefit plan does not provide coverage for compounded medications. Please ... medication with a dot under the step therapy column. Some plans may have step therapy programs on additional
Prescription Drug Guide October 2021
www.myprime.comPrescription drugs are classified as either a Brand drug or a Generic drug. The Brand or Generi c status provided is by a nationally recognized company providing drug product information. The Brand/Generic status for a specific drug/specific marketer can sometimes change over the life of a product in the marketplace and change from
Prescription, Drug, Generic, Negeri, Prescription drug, Generic drugs, Ge neric
SourceRx 1.0 Four Tier Prescription Drug List, October 2021
www.myprime.comSourceRx 1.0 Four Tier Prescription Drug List, October 2021 II Member Prescription Benefit The prescription benefit is multi-tiered, placing prescription drugs into one of four tier levels. Tier 1 primarily contains preferred (lowest cost) generic drugs. Based on cost considerations , there may be brands placed into this tier on occasion as well.
Prescription, Four, Tier, Sourcerx 1, Sourcerx, 0 four tier prescription
Blue Cross and Blue Shield of Kansas Formulary for ...
www.myprime.comBlue Cross and Blue Shield of Kansas (BCBSKS) complies with applicable Federal civil rights laws and does not discriminate on the basis of race, color, national origin, age, disability, or sex. BCBSKS does not exclude people or treat them differently because of race,
Health Insurance Marketplace 6 Tier Drug List
www.myprime.comBCBSIL Health Insurance Marketplace 6 Tier Drug List January 2022 IV ACA Preventive (ACA): Medicines marked in the ACA column are under the Affordable Care Act coverage of preventive services. These products have limited or $0 member cost-sharing (copay or co-insurance), when
BCBSTX Health Insurance Marketplace 6 Tier Drug List ...
www.myprime.comShoppers: To find drug estimates go to https://www.myprime.com/en/plan-preview/medicines/find-medicine.html Members: Log in to your plan to find current drug pricing ...
Rx90 (Maintenance) Drug List Effective January 1, 2021
www.myprime.comamlodipine besylate tab 10 mg (base equivalent) (Norvasc) amlodipine besylate-benazepril hcl cap 2.5-10 mg amlodipine besylate-benazepril hcl cap 5-10 mg (Lotrel) amlodipine besylate-benazepril hcl cap 5-20 mg (Lotrel) amlodipine besylate-benazepril hcl cap 5-40 mg amlodipine besylate-benazepril hcl cap 10-20 mg (Lotrel)
MEDICARE PART D TIER EXCEPTION INFORMATION
www.myprime.comFax: 800-693-6703 Phone: 800-693-6651 Please read all instructions below before completing the attached form. • Please complete the attached Request for a Lower Copay* (Tier Exception Form) • To prevent delays in the review process please complete all requested fields. • Completed forms should be faxed to: 800-693-6703
Blue Cross and Blue Shield of Alabama Source+Rx 1.0 ...
www.myprime.comAffordable Care Act Drugs marked with a dot in the ACA column may have limited or $0 member cost-sharing under the Affordable Care Act if certain criteria are met. Examples of categories of drugs that may be subject to limited or $0 member cost share include aspirin, breast cancer prevention drugs, fluoride supplements, folic acid supplements,
Capital Health Plan NetResults Formulary
www.myprime.comclinical or cost advantage over non-preferred drugs within the same therapeutic category. Coverage and copayment/co-insurance levels vary depending on the plan. Drugs that require Prior Authorization, Step Therapy, or that have Dispensing Limits or are considered Limited Distribution are noted in the Prescription Drug List. Limitations
Related documents
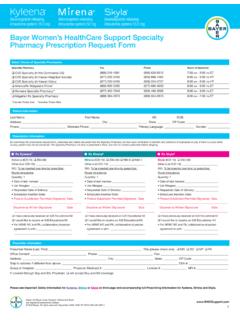
Bayer Women’s HealthCare Support Specialty Pharmacy ...
www.whcsupport.comThe Specialty Pharmacy Program prescription process To order Kyleena, Mirena or Skyla, complete the Specialty Pharmacy Prescription Request Form as follows: 1. Select Specialty Pharmacy. 2. Enter the patient and prescriber information in the space provided on the Specialty Pharmacy Prescription Request Form, including the patient’s pharmacy ...
508C, Specialty Pharmacy Network
www.bcbst.comSpecialty Pharmacy Network The pharmacies in our Specialty Pharmacy Network provide our members with self-administered and provider-administered specialty drugs at discounted rates. When your doctor sends your prescription to the specialty pharmacy, they’ll send your drugs to your home or provider’s office.
Network, Specialty, Pharmacy, Network specialty pharmacy, Specialty pharmacy
Participating Retail Pharmacies
www.caremark.comCurascript Pharmacy CVS Caremark Specialty Pharmacy CVS/Longs CVS/pharmacy D Dahl’s Pharmacy Dierbergs Pharmacy Dillon Pharmacy Discount Drug Mart Doc’s Drugs Doctor’s Choice Pharmacy Dominick’s Pharmacy Drug Town Pharmacy Drug Warehouse Drug World Drugs for Less Duane Reade Duluth Clinic E EPIC Eaton Apothecary Econofoods F
2020 Specialty Pharmacy Trend Report - AcademyNet
academynet.com3 As the specialty pharmacy market expands, LHS are re-evaluating growth strategies and the degree to which pharmacy services are integrated into care pathways. LHS continue to examine strategic plans for specialty pharmacy based on internal core competencies, the competitive landscape within their geographical markets, and patient/payer mix.
Botox CCRD Prior Authorization Form
static.cigna.comCigna’s nationally preferred specialty pharmacy **Medication orders can be placed with Accredo via E-prescribe - Accredo (1640 Century Center Pkwy, Memphis, TN 38134-8822 | NCPDP 4436920), Fax 888.302.1028, or Verbal 866.759.1557
Open Medication Guide - Florida Blue
www.bcbsfl.comSpecialty Medications: Covered Specialty Medications as indicated in the Medication List . Condition Care Rx* Value/HSA Preventive Prescription Medications: Refer to the Condition Care Rx Program section of this Medication Guide for a description of the program . Medications that are not covered Your pharmacy benefit may not cover select ...
Guide, Medication, Florida, Specialty, Blue, Pharmacy, Medication guide, Florida blue
Specialty Pharmacy Drug List - Magellan Rx Management
magellanrx.comSpecialty medications may be covered under either the medical or pharmacy benefit. Please consult your insurance documentation to determine which benefit covers these medications. We offer a broad specialty medication list containing nearly 500 drugs, covering 42 therapeutic categories and specialty disease states.
Specialty pharmacy requirements - UHCprovider.com
www.uhcprovider.comSpecialty pharmacy requirements For UnitedHealthcare commerical plan members PCA-1-21-04577-PH-WEB_12152021 Medication sourcing requirement — all outpatient providers. Places of service: Outpatient facility, physician office, home, ambulatory infusion . To support the provider/patient relationship in managing rare and complex chronic ...
FastStart New Prescription Fax Form - Caremark
www.caremark.comIf you would like to send a maintenance prescription to CVS Caremark Mail Service Pharmacy for your patient, please complete this form and fax it to the number above or ePrescribe (see step 4). Fax # 1-800-378-0323 Step 3: Physician Information Required