#407: Appropriate Treatment of MSSA Bacteremia
the measure based on the services provided and the measure-specific denominator coding. Measure Reporting: The listed denominator criteria is used to identify the intended patient population. The numerator options included in this specification are used to submit the quality actions allowed by the measure. The quality-data codes listed do not ...
Tags:
Information
Domain:
Source:
Link to this page:
Please notify us if you found a problem with this document:
Documents from same domain
Quality ID #236: Controlling High Blood Pressure
qpp.cms.govQuality ID #236: Controlling High Blood Pressure – National Quality Strategy Domain: Effective Clinical Care – Meaningful Measure Area: Management of Chronic Conditions. 2021 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Intermediate Outcome – High Priority . DESCRIPTION:
Quality ID #154 (NQF: 0101): Falls: Risk Assessment ...
qpp.cms.govQuality ID #154 (NQF: 0101): Falls: Risk Assessment – National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process This is a two-part measure which is paired with Measure #155: Falls: Plan of Care. If the falls risk assessment
Quality ID #154 (NQF: 0101): Falls: Risk Assessment
qpp.cms.govFoundation (PCPI®) and the National Committee for Quality Assurance (NCQA). These Measures are not a clinical guideline and does not establish a standard of medical care, and has not been tested for all potential applications. The Measures, while copyrighted, can be reproduced and distributed, without modification, for noncommercial
Fall, Assessment, Quality, Risks, Assurance, 1010, Risk assessment, Quality assurance
Quality ID #323: Cardiac Stress Imaging Not Meeting ...
qpp.cms.gov#323: Cardiac Stress Imaging Not Meeting Appropriate Use Criteria: Routine Testing After Percutaneous Coronary Intervention (PCI) Please refer to the specific section of the Measure Specification to identify the denominator and numerator
Quality ID #134 (NQF 0418): Preventive Care and Screening ...
qpp.cms.govQuality ID #134 (NQF 0418): Preventive Care and Screening: Screening for Depression and Follow-Up ... (6.6 percent) adults aged 18 or older had at least one MDE in the past year, with 10.2 million adults (4.3 percent) having one MDE with severe . impairment in the past year (Center for Behavioral Health Statistics and Quality, 2015). Data ...
Screening, Care, Preventive, Depression, 1048, Screening for depression, Nqf 0418, Preventive care and screening
Measure #324: Cardiac Stress Imaging Not Meeting ...
qpp.cms.gov2009 Appropriate Use Criteria for Cardiac Radionuclide Imaging Indication 12: Detection of CAD/Risk Assessment Without Ischemic Equivalent: Asymptomatic: Low CHD risk (ATP III risk criteria) - Inappropriate (1) 2006 Appropriateness Criteria for CCT and CMR Indication 10 - Detection of CAD: Asymptomatic (Use of CCTA)
Quality ID #46 (NQF 0097): Medication Reconciliation Post ...
qpp.cms.govMedication reconciliation post-discharge is an important step to catch potentially harmful omissions or changes in prescribed medications, particularly in elderly patients that are prescribed a greater quantity and variety of medications (Leape, 1991). Although the magnitude of the effect of medication reconciliation alone on patient
Quality ID #134: Preventive Care and Screening: Screening ...
qpp.cms.govDementia (CSDD), PRIME MD-PHQ-2, Hamilton Rating Scale for Depression (HAM-D), Quick Inventory of Depressive Symptomatology Self-Report (QID-SR), Computerized Adaptive Testing Depression Inventory (CAT-DI), and Computerized Adaptive Diagnostic Screener (CAD-MDD) • Perinatal Screening Tools
Screening, Care, Preventive, Dementia, Preventive care and screening
Quality ID #1 (NQF 0059): Diabetes: Hemoglobin A1c (HbA1c ...
qpp.cms.govGalantamine Rivastigimine. Miscellaneous central nervous system agents . Memantine. OR Most Recent Hemoglobin A1c Level > 9.0% . Performance Met: CPT II 3046F: Most recent hemoglobin A1c level > 9.0% . OR Hemoglobin A1c not Performed, Reason not Otherwise Specified
Quality ID #130 (NQF 0419): Documentation of Current ...
qpp.cms.gov*Signifies that this CPT Category I code is a non-covered service under the Medicare Part B Physician Fee Schedule (PFS). These non-covered services should be counted in the denominator population for MIPS CQMs. Denominator Criteria (Eligible Cases): Patients aged ≥ 18 years on date of encounter . AND
Related documents
Skilled Nursing Facility Quality Reporting Program Measure ...
www.cms.govSNF QRP Measure Calculations and Reporting User’s Manual V3.0 – Effective: October 1, 2019 1 Chapter 1 Skilled Nursing Facility Quality Reporting Program Measure Calculations and Reporting User’s Manual Organization and Definitions The purpose of this manual is to present the methods used to calculate quality measures that are
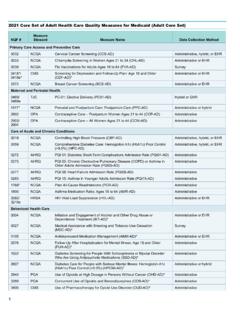
2021 Core Set of Adult Health Care Quality Measures for ...
www.medicaid.gov* This measure is no longer endorsed by NQF. ** The Adult Core Set includes the NCQA version of the measure, whichis adapted from the CMS measure (NQF #1879). *** AHRQ is the measure steward for the survey instrument in the Adult Core Set (NQF #0006) and NCQA is the developer of the survey administration protocol. ˄
2020 Shared Savings Program Quality Measure Benchmarks
www.cms.govThe quality measure benchmarks were calculated using ACO, group practice, and individual physician data aggregated to the practice or taxpayer identification number (TIN) level. These calculations only include a practice or TIN’s data if it had at least 20 cases in the denominator
Programs, Quality, Measure, Savings, Benchmark, Shared, Quality measures, Shared savings program quality measure benchmarks
Construction Quality Assurance/Quality Control Plan ...
images.template.netQuality (ODEQ), signed 31 October 2008 (DEQ No. LQVC-NWR-08-04). The purpose of this document is to present the CQA/QC requirements for construction of the Groundwater Source Control Measure (GW SCM)
U. S. Department of Health and Human Services Health ...
www.hrsa.govare designed to measure systems of care and are derived from clinical or practice guidelines. Data that is defined into specific measurable elements provides an organization with a meter to measure the quality of its care. Performance . measurement. is a process by which an organization monitors important
COMPETENCY STANDARDS - A MEASURE OF THE QUALITY …
www.isprs.orgCOMPETENCY STANDARDS - A MEASURE OF THE QUALITY OF A WORKFORCE John C Trinder School of Surveying and SIS, The University of New South Wales, UNSW SYDNEY NSW 2052, Australia Commission VI, WG VI/5 KEY WORDS: Capacity Building, Joint Education, Photogrammetry, Remote Sensing, Geoinformation Management, Skills Formation ABSTRACT:
PROFESSIONAL QUALITY OF LIFE SCALE (PROQOL)
proqol.orgProfessional Quality of Life: Compassion Satisfaction and Fatigue Version 5 (ProQOL). www.proqol.org. This test may be freely copied as long as (a) author is credited, (b) no changes are made, and (c) it is not sold. ... because scientifically the measure ...
Quality, Professional, Life, Measure, Professional quality of life
Sepsis Core Measure Checklist - IHA
www.ihaconnect.orgSepsis Core Measure Checklist Date of Admission: _____ (Time Zero= Time at which infection is identified/documented + 2 SIRS present with 6 hours of one another) ED Team ... Gina Croxford in the Quality Department. Not a part of the permanent medical record, DO NOT SCAN.
FLEXURAL STRENGTH – A MEASURE TO CONTROL …
www.ijser.orgAbstract- Flexural strength is a measure of the tensile strength of an unreinforced concrete beam or slab to resist failure in bending. It is useful in knowing the quality of concrete work done in road construction. Because of low initial cost, flexible roads are preferred, to concrete road pavement, but b roads getsituminous deteriorated ...
Quality, Control, Measure, Strength, Flexural, Flexural strength a measure to control
Quality ID #134: Preventive Care and Screening: Screening ...
qpp.cms.govMeasure data may be submitted by individual MIPS eligible clinicians, groups, or third party intermediaries. The listed denominator criteria are used to identify the intended patient population. The numerator options included in this specification are used to submit the quality actions as allowed by the measure. The quality-data codes listed do not
Quality, Screening, Care, Measure, Preventive, Preventive care and screening