Adjustment codes and coordination of benefits (COB)
secondary claims to provide information on a previous payer’s payment. If the previous payer sent a Health Insurance Portability and Accountability Act (HIPAA) standard 835 electronic remittance advice (ERA), you’ll see these codes in the ERA. Just transfer them to your secondary claim…
Download Adjustment codes and coordination of benefits (COB)
Information
Domain:
Source:
Link to this page:
Please notify us if you found a problem with this document:
Documents from same domain
Find out how members can save on lab costs - Aetna
www.aetna.com• Accu Reference Medical Laboratory, LLC • Advanced Clinical Laboratory Solutions, Inc. • Alere Toxicology • Ameritox • ARL/Labsouth, Inc.
Coverage of Experimental and Investigational …
www.aetna.comCoverage of Experimental and Investigational Procedures Policy Aetna covers experimental or investigational technologies (i.e., …
Aetna, Procedures, Coverage, Experimental, Investigational, Coverage of experimental and investigational, Coverage of experimental and investigational procedures
Aetna OfficeLink Updates - All regions September …
www.aetna.comSeptember 2017 Aetna OfficeLink Updates™ All regions Inside this issue Updates to our precertification list 2 Clinical payment, coding and policy updates 3 – 4
2017, Aetna, September, Aetna officelink, Officelink, September 2017 aetna officelink
How to use electronic referrals - Aetna
www.aetna.comSpecialty family Aetna specialties Taxonomy code GASTROENTEROLOGY Colon and rectal surgery Gastroenterology Gastroenterology (pediatric) Hepatology Proctology 207RG0100X GENERAL PRACTICE Adolescent medicine Developmental medicine
PLAN DESIGN AND BENEFITS PROVIDED BY …
www.aetna.comCustom Medicare HMO Open Access Plan State of New Jersey PLAN DESIGN AND BENEFITS Aetna Medicare SM Plan (HMO) PROVIDED BY AETNA HEALTH INC Arizona, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Maryland, Maine, New
States, Design, Aetna, Benefits, Plan, Provided, Plan design and benefits provided by
Great Savings on Hearing Aids - Aetna
www.aetna.comGreat Savings on Hearing Aids! Hearing loss is the third most prevalent medical condition among Americans over age 65 after arthritis and hypertension.
Aetna, Savings, Aids, Hearing, Great savings on hearing aids, Great
You don’t join us, we join youSM - Aetna
www.aetna.comOur Code of Conduct is grounded in and reflects the principles at the heart of The Aetna Way. The Code guides our compliance with the rules and regulations that govern our business throughout the world.
Volume 10, Issue 1 Aetna OfficeLink Updates
www.aetna.comQuality health plans & benefits Healthier living Financial well-being Intelligent solutions March 2013 • Volume 10, Issue 1 Mid-America Region
Aetna, Volume, 2013, Issue, March, Volume 10, Issue 1 aetna, March 2013, Issue 1
Ptosis Surgery Precertification Information …
www.aetna.comPCFX . Ptosis Surgery Precertification Information Request Form . About this form . You can’t use this form to initiate a precertification request.
Form, Information, Request, Surgery, Precertification, Ptosis, Ptosis surgery precertification information, Ptosis surgery precertification information request form
A quick reference guide for health care …
www.aetna.comQuality health plans & benefits Healthier living Financial well-being Intelligent solutions. A quick reference guide for health care professionals
Health, Guide, Reference, Care, Quick, Quick reference guide for health care
Related documents
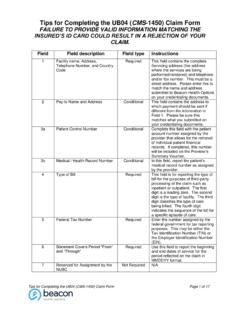
Tips for Completing the UB04 (CMS-1450) Claim Form
www.valueoptions.comTips for Completing the UB04 (CMS-1450) Claim Form FAILURE TO PROVIDE VALID INFORMATION MATCHING THE INSURED’S ID CARD COULD RESULT IN A REJECTION OF YOUR CLAIM. Tips for Completing the UB04 (CMS-1450) Claim Form Page 1 of 17 ... primary, secondary and tertiary payer through which the coverage is provided to the member. Tips for Completing ...
American Dental Association Claim Form
hr.cornell.eduWhen a claim is being submitted to the secondary payer, complete the entire form and attach the primary payer’s Explanation of Beneits (EOB) showing the amount paid by the primary payer. You may also note the primary carrier paid amount in the “Remarks” ield (Item 35). There are additional detailed completion instructions in the CDT manual.
Elementary and Secondary School Emergency Relief Fund
oese.ed.govfund/elementary-secondary-school-emergency-relief-fund/. If you have questions that are not answered in this document, please e-mail ESSERF@ed.gov. 1 The Coronavirus Aid, Relief, and Economic Security Act (CARES Act), Public Law 116-136, 134 Stat. 281 (Mar. 27, 2020). All citations in this document are to the CARES Act, unless otherwise indicated.
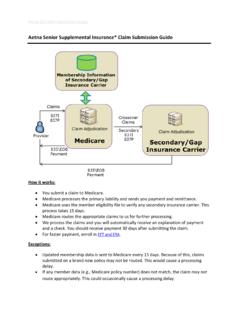
Aetna Senior Supplemental Insurance* Claim Submission Guide
www.aetnaseniorproducts.com• Since Medicare automatically routes secondary claims to us, 96% of those paper claims turn out to be unnecessary duplicates. • Following the steps above before submitting a paper claim will help you avoid wasting time and money. *Aetna Senior Supplemental Insurance owns and/or administers the following companies.
Category A and B Biological Agents
www.cdc.gov161 Public Health Preparedness: Mobilizing State by State Category A Agents The U.S. public health system and primary healthcare providers must be prepared to address various
CLAIM TIMELY FILING POLICIES
www.cigna.comCLAIM TIMELY FILING POLICIES To ensure your claims are processed in a timely manner, please adhere to the following policies: INITIAL CLAIM – must be received at Cigna-HealthSpring within 120 days from the date of service. SECONDARY FILING – must be received at Cigna-HealthSpring within 120 days from the date on the Primary Carrier’s EOB.
Policies, Claim, Filing, Secondary, Cigna, Timely, Claim timely filing policies
Medicare Secondary Payer (MSP) Manual
www.cms.gov2. If the contractor receives a claim for secondary benefits and could, without further development (for example, the EOB from another insurer or third party payer contains all necessary data), add an MSP occurrence and pay the secondary claim, it submits a validity indicator of "I" to add any new MSP occurrences (only if no MSP
Billing for Services when Medicare is a Secondary Payer
www.cms.govFeb 23, 2021 · Liability (L), No-Fault (NF) or Workers’ Compensation (WC) Medicare Secondary Payer (MSP) record on the beneficiary’s Medicare file or if a claim was inappropriately denied. You must continue to see or provide services to the beneficiary. If services relate to an open MSP accident or injury incident, first bill the other insurer as primary.
Services, Medicare, Claim, Billing, When, Secondary, Payer, Billing for services when medicare is a secondary payer
affidavit for death benefit claim - sss.gov.ph
www.sss.gov.phTitle: affidavit for death benefit claim Author: mikey Subject: affidavit for death benefit claim Created Date: 191040602141707
UFT/RTC Supplemental Health Insurance Program (SHIP)
www.uft.orgALL health plan(s) including Long Term Care (LTC) are primary to SHIP except NYSUT Catastrophic, which is secondary to SHIP. Listed Below are the document(s) required and limitations to process a claim, see SHIP brochure for further details. All claims require: Item a. SHIP Claim Form which “MUST” be signed and completed. 1.