Search results with tag "Payer"
Aetna Payer Sheet
www.aetna.comon all claims and reversals. The following is a summary of our new requirements. The items highlighted in the payer ... 341-HB Other Payer Amount Paid Count Max of 9 RW Required when Other Payer Amount Paid Qualifier (342-HC) is used 342-HC Other Payer Amount Paid
CVS CAREMARK PAYER SHEET
www.caremark.comPayer/Processor Name: CVS Caremark® Plan Name/Group Name: All Effective as of: January 2Ø21 ... 3Ø9-C9 Eligibility Clarification Code RW Submitted when requested by ... 34Ø-7C Other Payer ID RW Required when identification of the Other Payer is necessary for
CHECKING ELIGIBILITY & PARTICIPANT IDENTIFICATION …
www.dhs.pa.govEligibility 01/05/2018 Benefi t Related En ty: Payer MEDICARE PART A Payer Iden fi er: 600 Message Text Recipient is dual eligible. Payment approval is subject to MA policy, service delivery rules and TPL. Status: Other or Addi onal Payor Eligibility 02/01/2018 Benefi t Related En ty: Payer TRANSFER PENALTY Payer Iden fi er: 903 Message Text
Provider Relations - Michigan
www.michigan.govProvider Relations Member Tab Navigating the Member tab within CHAMPS ... This section provides the patient pay amount for nursing facility, hospice or inpatient care . Member Tab – 2/20/18 ... The name of the payer Payer ID: This is the CHAMPS Payer ID …
MEDICARE PARTS A, B, AND DMERC CONTRACTOR PAYER ID
provider.indianamedicaid.comMEDICARE PARTS A, B, AND DMERC CONTRACTOR PAYER ID . Table 1 – Medicare Part A Contractor Payer IDs . Medicare
ERA Payer List for UnitedHealthcare, Affiliates and ...
www.uhcprovider.comEDI: Electronic Remittance Advice (ERA/835) Payer List for UnitedHealthcare Affiliates and Strategic Alliances Author: kalle44 Subject: Listing of Payer ID by State and Brand/Plan Name Created Date: 8/21/2019 9:33:44 AM
OptumRx NCPDP Version D.0 Payer Sheet COMMERCIAL …
professionals.optumrx.comNCPDP Version D.0 Payer Sheet COMMERCIAL AND MEDICAID Payer Name: OptumRx Date: 05/01/2021 Commercial and Medicaid BIN: 610494 PCN: 9999 Community Health BIN: 610613 PCN: 2417 ProAct BIN: 017366 PCN: 9999 FlexScripts/ProAct BIN: 018141 PCN: 9999 United Healthcare Community Plan of Indiana BIN: 610494 PCN: 4841 ...
SAICA GUIDANCE REMOVING AND ADDING TAXPAYER …
saicawebprstorage.blob.core.windows.netSARS will check if you if have ‘Manage Payer Rights’ on both the requesting and holding portfolio. Once verified the tax type will be transferred immediately. c) Where the owner or registered representative does not approve the ... As part of the authentication process, you will be required to enter a One-Time-Pin (OTP).
Chapitre 6 - Les effets de commerce
www.escem.rnu.tnun effet à payer et pour le bénéficiaire, un effet à recevoir. 1.2. Les caractéristiques de la traite ou de la lettre de change La lettre de change contient des mentions obligatoires et d'autres facultatives : - la date de création, - la date de règlement (échéance), - la somme à payer inscrite en lettres et en chiffres, - le nom du ...
Bind On-Demand Health Insurance Administrative Guide
www.uhcprovider.comBind Benefits, Inc., is the payer ID: 25463. Bind Benefits, Inc., may be entered as the “insurance” carrier (dependent on provider processing system). This payer ID may be attached to multiple networks. Examples include: • UHC networks • PreferredOne network (through 2020) • SmartHealth network Refer to the member ID card
California Department of Health Care Services (Medi-Cal Rx ...
medi-calrx.dhcs.ca.govOct 22, 2020 · NCPDP Standard Payer Sheet . Version 1.0 . October 22, 2020 . Instructions Related to Transactions Based on NCPDP Version D.0 (B1) Claim Billing (B2) Claim Reversal (B3) Claim Rebill (P2) Prior Authorization Reversal (P3) Prior Authorization Inquiry (P4) Prior Authorization Request . Note:
Instructions on how to fill out the CMS 1500 Form
www.lacare.orgDETERMINE WHETHER MEDICARE IS THE PRIMARY OR SECONDARY PAYER. If there is insurance primary to Medicare for the service date(s), enter the insured’s policy or group number within the confines of the box and proceed to items 11a–11c. Items 4, 6, and 7 must also be completed. If item 11 is left blank, the claim will be denied as unprocessable.
PSI 90 Fact Sheet - Agency for Healthcare Research and Quality
qualityindicators.ahrq.govall-payer reference population. In the modified version of PSI 90 (v6.0), weighting of the individual component indicators is based on two concepts: the volume of the adverse event and the harm associated with the adverse event. The volume weights were calculated based on the number of safety-related
Extra-Statutory Concessions - GOV.UK
assets.publishing.service.gov.ukagreement: payer resident abroad A13. Administration of estates: deficiencies of income allowed against income of another year A14. Deceased person's estate: residuary income received during the administration period A15. Dependent relative allowance A16. Annual payments (other than interest) paid out of income not brought into charge to income tax
2021 Coding & Payment Quick Reference - Boston Scientific
www.bostonscientific.com1. 2021 Coding & Payment Quick Reference. Select Laparoscopic Cholecystectomy Procedures with and without Common Bile Duct Exploration (CBDE) Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements.
Working Aged - Centers for Medicare & Medicaid Services
www.cms.govSlide 3 - of 25 - Course Overview . Slide notes . This course will provide an overview of the MSP provisions of the Social Security Act for beneficiaries entitled to Medicare based on age, provide guidelines for the small employer exception, provide examples showing when Medicare would be the secondary payer, and provide
Understanding Patient Limit275 - SAMHSA
www.samhsa.gov5) Accepts third-party payment for some services, though not necessarily for buprenorphine-related services and not necessarily all third-party payers. What is the process to request a patient limit of 275? Eligible practitioners who want to increase their patient limit to 275 must submit a completed
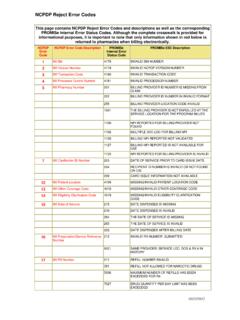
NCPDP Reject Error Codes - Department of Human Services
www.dhs.pa.govPROMISe ESC Description 1 M/I Bin 4178 INVALID BIN NUMBER 2 M/I Version Number 4179 INVALID NCPCP VERSION NUMBER ... Primary Payer 2532 TPL PAYMENT AMOUNT IS BEING USED FOR REPORTING PURPOSES 50 Non-Matched Pharmacy Number 1000 BILLING PROVIDER ID NOT ON FILE
Conditional Payment Letters and Conditional Payment …
www.cms.govfor services where another payer may be responsible. This conditional payment is made so that the Medicare beneficiary won’t have to use their own money to pay the bill. The payment is “conditional” because it must be repaid to Medicare when a settlement, judgment, award or other payment is secured.
Disputing A Claim - Centers for Medicare & Medicaid …
www.cms.govWelcome to the Medicare Secondary Payer Recovery Portal (MSPRP) Disputing a Claim course. As a reminder, you may view the slide number you are on by clicking on the moving cursor. Additionally, you can view the narration by clicking the [CC] button in the lower right-hand corner of the screen.
Reimbursements–Tax Dilemmas Explained
www.pwc.inthat the payer has the obligation to withhold tax on the gross amount. 1. Sections 192 to 194LD, Section 194H 2. DCIT vs Zee Entertainment Enterprises Ltd (Bombay High Court) 3. Section 194C, 194J, 194DA, 194EE,194F,194-IA,194-IC and 194LA 4. …
CPT® and ICD-9 are dictated by payer policy guidelines ...
asmbs.orgJan 01, 2012 · Importantly, these 2013 coding changes involve only the psychotherapy codes – the codes found in the Psychiatry section of the 2013 CPT® manual. There are no changes to other codes that psychologists use, such as testing or health and behavior codes. Bariatric ICD-9-CM Diagnostic Codes by Body System Cardiovascular System
Tax Year 2021 W-2c Online Tutorial
www.ssa.govTax Year 2021 W-2c Online Tutorial . TY21 W-2c Online Tutorial . Page 2 . ... and select the Kind of Payer and the Kind of Employer, then select the Continue button to go to the “Enter W-2c Information” page. • Select the Cancel button to return to the EWR home page.
UnitedHealthcare Medicare Advantage administrative changes ...
www.uhcprovider.comPlease remember to check the member’s updated ID card. To reflect the plan and administrative changes outlined here, we’ll update the 2022 member ID cards with the new Payer ID and contact information. Verify member eligibility Verify member eligibility at the time of service online, using electronic data interchange (EDI) or by phone.
Part 4 Billing - Indian Health Service
www.ihs.gov3.3 Medicare Secondary Payer (MSP) 3.4 Medicare Timely Filing 3.5 Claims Resubmission Guidelines 3.6 Reimbursement for Clinical Nurse Specialist (CNS), Nurse Practitioner (NP), and Physician Assistant (PA) 3.7 Medicare Resources 4. Billing Medicaid 4.1 About Medicaid Billing 4.2 Medicaid Approval and Export Process 4.3 Medicaid Timely Filing 5 ...
Medicare Secondary Payer Recovery Process
www.cms.govrecovery case unless you tell us to do so. If you have a representative, BCRC will need a signed Proof of Representation or Authorization. Authorizations must include: n The name of the attorney/law frm or other representative n Your name, printed n …
Reporting a Case to the BCRC - Centers for Medicare ...
www.cms.govresearch Medicare Secondary Payer (MSP) situations, as appropriate. (e.g., They collect the information from claims processors, MMSEA Section 111 Mandatory Insurer Reporting submissions, workers’ compensation entities) • The BCRC is responsible for updates to MSP situations, including insurance updates, address changes, changes
Off-payroll working rules (IR35) flowchart for contractors
assets.publishing.service.gov.ukintermediary (usually the fee-payer) will deduct tax and National Insurance Contributions (NICs) before they pay for your services. You will still need to submit a tax return, but relief is available on the tax already paid. If you disagree with the status determination by your client, you can dispute the decision with them.
Secure Acceptance Checkout API Integration Guide
developer.cybersource.comSecure Acceptance Checkout API Integration Guide | 4 Contents Configuring Payer Authentication 23 Enabling Automatic Authorization Reversals 24 Enabling Echecks 25 Enabling PayPal Express Checkout 25 Security Keys 26 Creating Security Keys 27 Merchant Notifications 28 Configuring Merchant Notifications 28 Customer Receipts 29 Configuring Customer …
MSP Laws and Third Party Payers Fact Sheet for Attorneys
www.cms.gov3. An itemized statement of attorney fees and procurement costs. 4. The name, address, and telephone number of the automobile or liability insurer involved, and if available, the policy number, claim number, and adjuster's name. 5. If monies are available through personal injury/med-pay or another form of
2021 Form 1099-MISC - IRS tax forms
www.irs.govGenerally, a payer must backup withhold if you did not furnish your TIN. See Form W-9 and Pub. 505 for more information. Report this amount on your income tax return as tax withheld. Box 5. Shows the amount paid to a fishing boat crew member who is considered by the operator to be self-employed. Self-employed individuals must
Claims Correction - CGS Medicare
www.cgsmedicare.comChapter 5 December 2019 CGS . Table of Contents ... FISS processes it through a series of edits to ensure the information submitted on the claim is complete and correct. If the claim has ... ability for providers to enter and correct Medicare secondary payer (MSP) claims and MSP adjustments via the FISS Direct Data Entry (DDE), in
National Uniform Claim Committee
nucc.orgFacility) 2310D (Supervising) 2300 NTE 2300 PWK 2310A REF01 ... HI11-2, HI12-2 22 2300 in the 837P Resubmission and/or Original Reference Number 2300 CLM05-3 Titled Claim Frequency Code in the 837P. REF02 Titled Payer Claim Control Number. 23 2300 2300 ... Rendering Provider ID # 2310B PRV03 REF02 Titled Provider Taxonomy Code and …
Qualified Health Information Network (QHIN) Technical ...
rce.sequoiaproject.orgThe healthcare provider is a participant in a health information network (state/local HIE, vendor- or payer-based, etc.), which is a Participant of a QHIN. To find health information about the patient, the provider first submits a Query Solicitation to the local network, which is routed to the QHIN over a secure channel. The
PAYER TYPE LIST PAYER PAYER TYPE TYPE CODE PAYER …
www.chiamass.govPayer Type & Payer Source Code List - Effective Date 10/01/09 7 174 Aetna Health Inc. - Quality POS 8 HMO 175 Aetna Health, Inc. - HMO 8 HMO 176 Carelink (CIGNA & Tufts) 7 COM 177 Chesapeake Life Insurance Company 7 COM 178 Children's Medical Security Plan (CMSP) 5 GOV 179 First Health Life and Health Insurance Company 7 COM
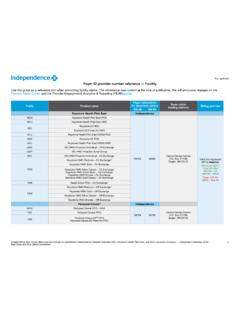
Payer ID provider number reference — Facility
www.ibx.comPayer ID provider number reference — Facility Rev. January 2022 2 Payer information Prefix Product name for electronic claims Emdeon payer information* Paper claim mailing address Billing provider ISA-08 GS-03 Personal Choice® (continued) Independence Valid and registered NPIReserve, is required. Electronic (837I) Loop 2010AA NM108 = XX
Payer Specification Sheet
www.primetherapeutics.comPage 1 of 17 Materials reproduced with the consent of © National Council for Prescription Drug Programs, Inc. 3851-D Payer Specification Sheet for Commercial Clients ...
Ability-to-Repay and Qualified Mortgage Rule
files.consumerfinance.govhomes and their employees what compensation must be ... Qualified Mortgages is that the borrower’s total debt- to-income ratio is not higher than 43 percent. For a temporary, transitional period, certain loans that are eligible for sale or guarantee by a
Ability-to-Repay and Qualified Mortgage Rule
files.consumerfinance.govrules (Sections 1, 2, and 2.2); Revised the section discussing verification of income under the general ATR standard tonote that a creditor is required to confirm that an inflow of funds into a consumer’s account are the consumer’s personal income if the creditor relies on those funds in making an ability-to-repay determination (Section
Ability-to-Repay & Qualified Mortgages
www.fdic.govAbility-to-Repay & Qualified Mortgages VI. What Charges Count Toward the QM Points and Fees Cap? 29 . FEDERAL DEPOSIT INSURANCE CORPORATION QM: Points and Fees Caps for 2016 Allowable Points Loan Amount Range* and Fees* $101,749 and up . 3% . $61,050 - $101,748.99 . $3,052 . $20,350 - $61,049.99 . 5% .
Ability-to-Repay and Qualified Mortgage Rule
files.consumerfinance.govAbility-to-Repay and Qualified Mortgage Rule Please refer to our concurrent proposal about the changes we have proposed to this rule. This notice proposes to amend the final rule issued January 10, 2013, which is set to take effect on January 10, 2014. The Bureau is considering comments received and plans to finalize the proposal as soon as ...
Similar queries
Aetna Payer Sheet, Claims, Payer, CAREMARK PAYER, Name, Caremark, Eligibility, Payer ID, Provider Relations, Michigan, Facility, Payer Payer ID, Contractor Payer, Payer List, Version, Payer Sheet, Authentication, California Department of Health Care, NCPDP Standard Payer Sheet, NCPDP Version D, Medicare, Secondary payer, Insurance, PSI 90 Fact Sheet, Extra-Statutory Concessions, 2021 Coding & Payment Quick Reference, Boston Scientific, Centers for Medicare & Medicaid Services, Overview, Party, Party payers, NCPDP Reject Error Codes, Conditional payment, Disputing a Claim, Centers for Medicare & Medicaid, Medicare secondary payer, Dilemmas Explained, Dictated by payer policy guidelines, Codes, W-2c Online Tutorial, Part 4 Billing, Indian Health Service, Process, Medicare Secondary Payer Recovery Process, Recovery, Off-payroll working rules, Secure Acceptance Checkout API, Payer Authentication, Third Party Payers Fact Sheet for Attorneys, Fees, IRS tax forms, CGS Medicare, Series, Reference Number, Number, Provider ID, Provider, LIST PAYER PAYER, List, Medical, Payer ID provider number reference — Facility, Sheet, National Council for Prescription Drug Programs, Ability-to-Repay, Qualified, Homes, Rules, To-Repay, FEDERAL DEPOSIT INSURANCE CORPORATION